Blog
How to Architect Scalable Vision Care Technology Platforms?

Modern vision care platforms must support connected diagnostic devices, AI-driven analytics, enterprise integrations, and regulatory compliance from day one. As ophthalmology and optometry products scale, architectural limitations quickly surface through performance bottlenecks, integration failures, and compliance gaps.
Scalability in vision technology is not achieved by adding servers. It requires intentional system design across device connectivity, cloud infrastructure, data pipelines, and regulatory-aligned development processes.
For companies building AI-powered retinal systems, eye tracking platforms, or enterprise ophthalmology software, architecture determines whether the product can scale securely and reliably.
Why Scalability Is Critical in Ophthalmology & Vision Care Platforms
Scalability in vision care technology is no longer a technical luxury; it is a commercial requirement.
Ophthalmology and optometry platforms today must process high-resolution retinal images, manage real-time diagnostic streams, integrate with enterprise systems, and maintain regulatory compliance simultaneously. As adoption grows across clinics, hospitals, and enterprise networks, system demands increase exponentially, not linearly.
For business decision-makers, scalability directly impacts revenue growth, valuation, and enterprise credibility.
1. The Explosion of Diagnostic Data
Modern ophthalmology platforms generate enormous volumes of structured and unstructured data:
- OCT scans produce detailed 3D retinal images
- Fundus photography in ultra-high resolution
- Visual field test datasets
- AI inference outputs
- Continuous eye-tracking data streams
According to the FDA’s Software as a Medical Device (SaMD) framework, AI-based diagnostic systems must maintain traceability, validation controls, and audit logs for clinical use (FDA SaMD Guidance: https://www.fda.gov/medical-devices/digital-health-center-excellence/software-medical-device-samd).
This means platforms must not only store and process data, but they must also do so in a compliant, auditable, and secure manner at scale.
Without a scalable cloud-native architecture:
- Image processing slows
- Storage costs balloon
- AI latency increases
- Clinical workflows are disrupted
For enterprise buyers, performance degradation equals lost trust.
2. Enterprise Healthcare Environments Demand Interoperability
Vision care platforms rarely operate in isolation. Enterprise customers expect seamless integration with:
- Epic
- Cerner
- Athenahealth
- Practice management systems
- Insurance billing platforms
FHIR-based interoperability standards from HL7 (https://www.hl7.org/fhir/) have become foundational for healthcare data exchange.
If your architecture does not support standardized APIs and scalable integration layers:
- Enterprise deployments stall
- Integration timelines extend
- Sales cycles lengthen
- IT security reviews fail
Scalable systems are API-first and integration-ready from day one.
For organizations building enterprise ophthalmology software, this architectural decision directly influences go-to-market velocity, and healthcare Software Development Expertise
https://citrusbits.com/healthcare-software-development/
3. AI Performance Degrades Without Scalable Infrastructure
AI-powered retinal systems and diagnostic platforms depend on consistent data throughput and compute elasticity.

Scalable AI infrastructure must support:
- Real-time inference for clinical workflows
- Batch training pipelines for model improvements
- Model version control and rollback
- Explainability frameworks for regulatory audits
- Data governance and bias monitoring
Without intentional AI architecture:
- Model drift goes undetected
- Inference latency disrupts clinic operations
- Compliance documentation becomes fragmented
- Clinical trust erodes
Scalability in ophthalmology AI is not just about compute; it is about governance, transparency, and operational resilience.
4. Regulatory Compliance Becomes More Complex at Scale
As vision platforms expand across regions and enterprise systems, regulatory obligations multiply:
- HIPAA (U.S.)
- GDPR (EU)
- FDA SaMD requirements
- SOC 2 audits
- State-level privacy laws
The U.S. Department of Health & Human Services outlines HIPAA Security Rule requirements for protecting electronic PHI (https://www.hhs.gov/hipaa/for-professionals/security/index.html).
At scale, manual compliance processes fail.
Architecturally mature platforms include:
- Role-based access control
- End-to-end encryption
- Continuous monitoring systems
- Automated audit logging
- Secure DevOps pipelines
Regulatory scalability is about embedding compliance into engineering workflows, not treating it as a post-launch add-on.
5. Scalability Directly Impacts Enterprise Valuation & Exit Potential
For venture-backed ophthalmology startups and device manufacturers, architecture affects more than performance; it affects valuation.
Investors and acquirers evaluate:
- Technical debt
- Infrastructure stability
- Security posture
- Regulatory readiness
- Multi-tenant scalability
A scalable, modular, cloud-native platform signals:
- Enterprise readiness
- Lower operational risk
- Expansion capability
- Long-term defensibility
Conversely, monolithic architecture limits growth and increases acquisition friction.
For B2B vision care companies, architectural maturity is a strategic asset.
Core Components of a Scalable Vision Care Architecture
Designing a scalable ophthalmology or vision care platform requires more than strong engineering talent; it demands architectural intentionality across devices, infrastructure, AI systems, interoperability, and compliance frameworks.
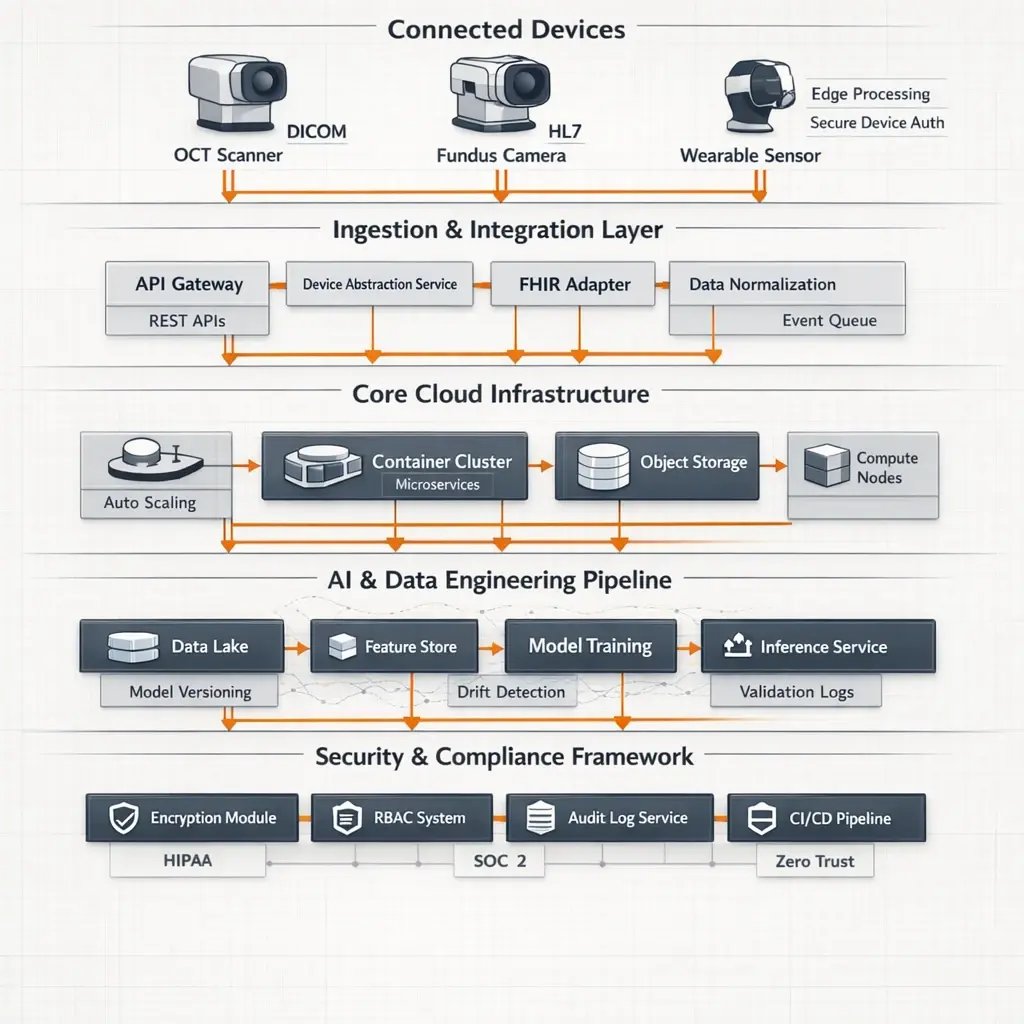
Below are the foundational components every enterprise-ready vision care platform must include.
1. Connected Diagnostic Device Integration Layer
Modern ophthalmology ecosystems rely on a growing network of connected diagnostic devices, including:
- Optical Coherence Tomography (OCT) systems
- Fundus cameras
- Visual field analyzers
- Corneal topographers
- Eye-tracking and wearable devices
Each device generates structured and unstructured clinical data in varying formats.
A scalable platform must include a device abstraction layer that standardizes data ingestion across multiple manufacturers and protocols.
Key architectural principles:
- Support for DICOM imaging standards (widely used in medical imaging)
- HL7 and FHIR compatibility for clinical data exchange (https://www.hl7.org/fhir/)
- Secure device authentication mechanisms
- Edge computing for preprocessing large imaging files
- Automated device onboarding workflows
Without abstraction, teams build one-off integrations, creating fragile systems that break as new devices are added.
Scalable platforms treat devices as modular inputs, not custom engineering projects.
For healthcare organizations building connected ecosystems, device integration strategy directly impacts deployment velocity.
2. Cloud-Native Infrastructure & Elastic Scalability
Vision care platforms process large imaging files, AI workloads, and multi-location user traffic. Traditional monolithic servers cannot support enterprise expansion.
Cloud-native architecture enables:
- Horizontal scaling under increased diagnostic demand
- Multi-region deployments for global clinics
- Disaster recovery and high availability
- Infrastructure-as-Code for predictable environments
- Containerized microservices (Docker, Kubernetes)
Elastic scalability ensures the system adapts automatically during:
- Peak clinic hours
- AI model training cycles
- Enterprise onboarding waves
However, scalability must also include cost optimization governance. Poor cloud architecture leads to uncontrolled compute expenses, particularly in AI-driven retinal analysis systems.
Enterprise buyers expect:
- 99.9%+ uptime
- Documented disaster recovery protocols
- SOC 2-aligned infrastructure controls
Cloud maturity signals operational reliability.
3. AI & Diagnostic Data Pipeline Architecture
AI-powered ophthalmology platforms require sophisticated data engineering beyond basic application logic.
Scalable AI systems must support:
- Real-time inference for diagnostic workflows
- Batch model retraining pipelines
- Secure model version control
- Clinical validation logging
- Explainability and bias auditing frameworks
Regulatory bodies increasingly emphasize transparency in AI-based healthcare systems. The FDA’s Software as a Medical Device (SaMD) framework outlines requirements for AI systems used in clinical decision support.
Without structured AI lifecycle management:
- Model drift goes unnoticed
- Regulatory documentation becomes fragmented
- Clinical trust declines
- Enterprise buyers hesitate
Scalable AI architecture separates:
- Data ingestion
- Feature engineering
- Model training
- Deployment pipelines
- Monitoring systems
This modular approach reduces risk while enabling continuous innovation.
4. Enterprise Interoperability & API-First Design
Ophthalmology platforms must integrate seamlessly with broader healthcare ecosystems.
Enterprise customers demand interoperability with:
- Electronic Health Records (EHRs)
- Practice Management Systems
- Insurance billing software
- Hospital IT infrastructure
FHIR-based APIs have become the industry standard for healthcare interoperability.
Scalable platforms adopt an API-first strategy that includes:
- Secure OAuth2-based authentication
- Tokenized access controls
- Data normalization services
- Audit-ready transaction logging
Failure to prioritize interoperability early leads to:
- Prolonged enterprise onboarding
- Costly integration retrofits
- IT security bottlenecks
- Lost sales opportunities
For B2B decision-makers, integration readiness directly influences enterprise adoption.
5. Security & Compliance by Architectural Design
Vision care platforms handle protected health information (PHI), diagnostic data, and AI outputs. Security must be foundational.
According to the U.S. Department of Health & Human Services, HIPAA Security Rule requirements mandate administrative, physical, and technical safeguards for ePHI.
Scalable architecture must include:
- End-to-end encryption (data in transit and at rest)
- Role-based access control (RBAC)
- Zero-trust security models
- Continuous monitoring & intrusion detection
- Immutable audit logs
- Secure CI/CD pipelines
As platforms expand across regions, compliance obligations increase (HIPAA, GDPR, FDA SaMD, SOC 2).
Embedding compliance into DevOps processes prevents regulatory bottlenecks later.
Learn more about secure digital health platform development: https://citrusbits.com/services/enterprise-platforms/
Common Architectural Mistakes That Limit Scalability in Vision Care Platforms
Even well-funded ophthalmology and vision tech companies encounter scalability roadblocks, not because of poor engineering talent, but because of early architectural shortcuts.
As platforms grow from pilot deployments to enterprise-scale adoption, foundational weaknesses surface quickly.
Below are the most common mistakes that limit scalability, and how forward-thinking organizations avoid them.
Building Monolithic Systems That Cannot Evolve
Many early-stage vision platforms are built as monolithic applications to accelerate MVP delivery. While this may reduce short-term development time, it creates long-term rigidity.
Monolithic systems often result in:
- Slower feature releases
- Increased deployment risk
- Limited horizontal scaling
- Tight coupling between device logic and backend systems
When diagnostic AI, imaging storage, user management, and integrations all live inside a single codebase, scaling becomes complex and expensive.
Modern scalable platforms adopt:
- Microservices architecture
- Containerization
- Independent service deployment
- Clear domain separation
This modularity allows AI components, imaging storage, and integrations to scale independently without disrupting clinical workflows.
Hard-Coded Device Integrations
Vision care platforms frequently integrate with OCT systems, fundus cameras, and visual field analyzers.
A common mistake is creating one-off, hard-coded integrations for specific manufacturers.
This leads to:
- Fragile integrations
- Long onboarding cycles for new devices
- High maintenance costs
- Vendor lock-in
Instead, scalable platforms implement:
- Device abstraction layers
- Standardized DICOM support
- HL7 and FHIR compatibility
- Secure, version-controlled device APIs
Organizations that fail to standardize device communication often struggle when expanding across multiple clinic networks.
Ignoring API-First Design
Enterprise healthcare buyers expect seamless interoperability.
Platforms that treat APIs as secondary considerations face:
- Integration bottlenecks
- Delayed enterprise contracts
- Security review failures
- Custom integration costs per client
API-first architecture ensures:
- Clean separation between frontend and backend systems
- Scalable third-party integrations
- Secure tokenized access control
- Faster enterprise deployment
Underestimating AI Lifecycle Governance
AI-powered retinal diagnostics and vision analytics platforms require structured lifecycle management.
Common AI scaling failures include:
- No model version tracking
- Lack of validation documentation
- Absence of explainability frameworks
- Unmonitored model drift
The FDA’s guidance on Software as a Medical Device (SaMD) highlights the importance of validation, documentation, and monitoring for AI-driven clinical systems.
Without governance:
- Regulatory audits become high-risk
- Clinical trust deteriorates
- Enterprise buyers hesitate
Scalable AI systems include:
- Model monitoring dashboards
- Controlled deployment pipelines
- Traceable audit logs
- Bias and performance monitoring
AI scalability is not just computational; it is regulatory and operational.
Treating Security & Compliance as Afterthoughts
One of the most expensive mistakes vision care companies make is retrofitting security and compliance after product-market fit.
At a small scale, gaps may go unnoticed. At enterprise scale, they become deal-breakers.
Common compliance oversights:
- Weak role-based access control
- Incomplete encryption practices
- Insufficient audit logging
- Manual compliance documentation
- Lack of SOC 2 alignment
The U.S. Department of Health & Human Services outlines strict safeguards required under the HIPAA Security Rule (https://www.hhs.gov/hipaa/for-professionals/security/index.html).
Security retrofits often result in:
- Costly architectural rework
- Delayed enterprise contracts
- Regulatory penalties
- Reputational risk
Scalable platforms embed compliance into DevSecOps processes from the beginning.
How to Future-Proof Your Vision Care Platform for Long-Term Growth
Architecting for today’s requirements is not enough. Vision care technology companies must design systems that support 3–5 years of clinical expansion, AI evolution, regulatory shifts, and enterprise demand.
Future-proofing a scalable ophthalmology platform requires strategic foresight across infrastructure, compliance, AI governance, and global readiness.
Adopt an API-First, Modular Architecture
Healthcare ecosystems are evolving rapidly. New devices, AI tools, payer systems, and interoperability standards continue to emerge.

An API-first strategy ensures your platform can:
- Integrate with future EHR systems
- Support third-party AI modules
- Enable partner ecosystems
- Launch new digital health services
- Expand into enterprise marketplaces
Modular microservices allow independent scaling of:
- Diagnostic processing
- Imaging storage
- User management
- Billing integrations
- AI model deployment
This architectural flexibility reduces refactoring risk as your product evolves.
Design for AI Evolution & Regulatory Adaptation
AI-driven retinal and diagnostic systems will not remain static. Models improve, regulations evolve, and explainability standards become stricter.
The FDA’s Digital Health Center of Excellence continues to refine guidance around AI/ML-based Software as a Medical Device (SaMD).
Future-proof AI architecture includes:
- Continuous learning frameworks with controlled updates
- Model performance monitoring dashboards
- Dataset version control
- Structured validation documentation
- Transparent explainability layers
Rather than treating AI as a fixed feature, scalable platforms treat it as an evolving clinical asset.
This reduces regulatory friction and builds long-term clinical credibility.
Prepare for Multi-Region Compliance & Data Governance
As ophthalmology platforms expand globally, compliance requirements multiply.
Organizations entering international markets must account for:
- HIPAA (U.S.)
- GDPR (EU)
- Regional health data residency laws
- Emerging AI transparency regulations
The European Commission outlines GDPR obligations for health data handling.
Future-ready platforms include:
- Multi-region cloud deployment capability
- Data localization controls
- Consent management systems
- Automated audit trail generation
- Configurable compliance frameworks
Scalable governance systems prevent regulatory slowdowns during expansion.
Implement Infrastructure Cost Governance Early
AI-driven imaging systems can quickly accumulate cloud costs due to:
- High-resolution image storage
- GPU-intensive inference workloads
- Continuous model training
Future-proof platforms incorporate:
- Automated scaling policies
- Storage lifecycle management
- Serverless event-driven processing
- Cloud usage monitoring dashboards
This ensures profitability scales alongside user growth.
Enterprise buyers evaluate long-term operational sustainability, not just technical capability.
Build for Enterprise Multi-Tenancy
As platforms expand across clinic networks, hospital systems, and enterprise buyers, multi-tenancy becomes critical.
Enterprise-grade architecture must support:
- Isolated tenant data environments
- Customizable workflows per organization
- Hierarchical user roles
- Secure cross-location access controls
- Centralized administrative dashboards
Without true multi-tenant architecture, scaling across enterprise clients becomes operationally inefficient.
Multi-tenancy enables:
- Faster enterprise onboarding
- Lower infrastructure duplication
- Scalable SaaS growth models
- Stronger recurring revenue frameworks
The Bottom Line
Architecting scalable ophthalmology and vision care platforms requires more than strong engineering; it demands strategic alignment between cloud infrastructure, connected diagnostic devices, AI governance, interoperability standards, and regulatory compliance from day one. For B2B healthcare leaders, scalability directly impacts enterprise adoption, operational efficiency, and long-term valuation.
Organizations that invest in intentional, future-ready architecture position themselves to grow securely and competitively in an increasingly AI-driven healthcare landscape. If you’re planning to scale a vision care or digital health platform, partner with an experienced healthcare technology team like CitrusBits to ensure your foundation is built for sustainable growth.
Table of Contents
1) Why Scalability Is Critical in Ophthalmology & Vision Care Platforms
2) Core Components of a Scalable Vision Care Architecture
3) Common Architectural Mistakes That Limit Scalability in Vision Care Platforms
4) How to Future-Proof Your Vision Care Platform for Long-Term Growth
5) The Bottom Line
Innovate the Future of Health Tech
CitrusBits helps MedTech leaders build smarter apps, connected devices, and XR health solutions that truly make an impact.
